Health in 2019: Humanitarian Emergency in the Dark
Even though the entry of humanitarian aid lit a spark of hope for the Venezuelan health system, the balance at the end of the year is anything but encouraging.
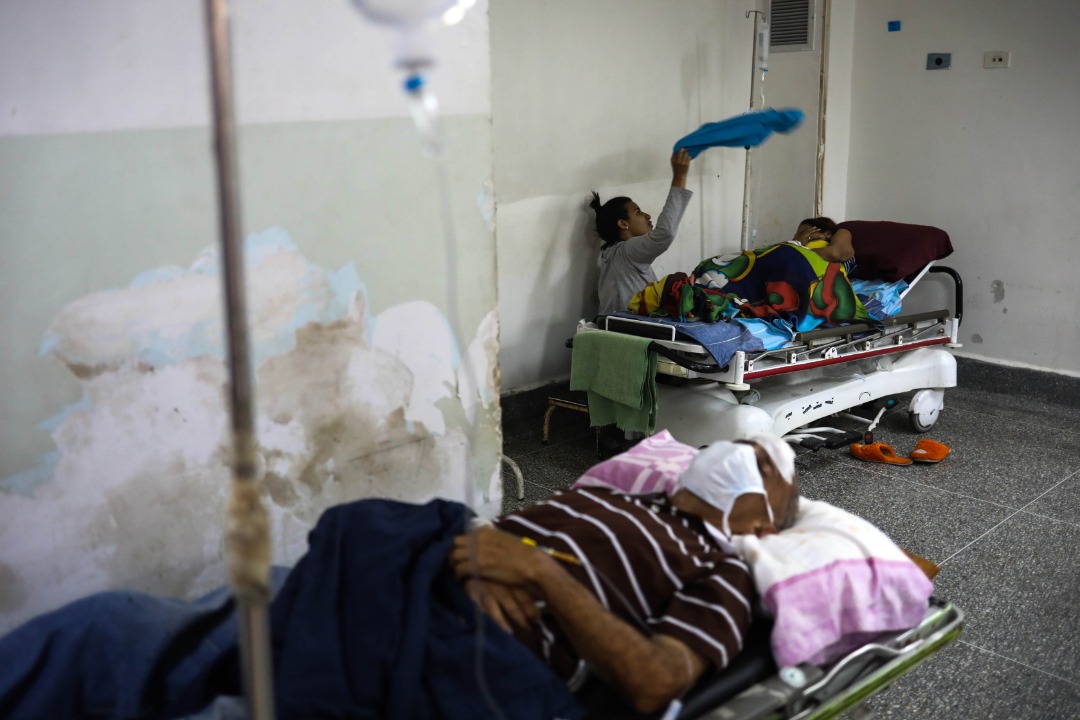
Photo: Cristian Hernández
With the enthusiasm that many Venezuelans experienced on January 23rd, Voluntarios por Venezuela, the network developed by the National Assembly to distribute the humanitarian aid donations, had a sudden rise of half a million volunteers. There was talk about shipments coming in from the borders, imminent change, rescuing the country.
Behind the future around the corner was the awareness of the disaster, built with hardships experienced daily, and with revelations from the first National Hospital Survey report this year. The numbers were terrifying: between November 19th, 2018 and February 9th, 2019, there were 1,557 deaths due to medical supplies shortage. Out of those, 79 were directly related to failures of the electrical system. And the nationwide blackout of March 7th hadn’t even happened.
The shortage of supplies was around 50% in ICUs and 35% in operation rooms.
Critical areas like ICUs, emergency rooms and ORs had intermittent operativity during the period studied. Since these areas were evaluated in hospitals that are national reference, any level below full operativity here meant that patients had to go to other states to receive treatment.
The shortage of supplies was around 50% in ICUs and 35% in operation rooms. In emergency rooms, there was no morphine or antihypertensives. What the survey found matches with the reality reported in a gazillion of places by people who require medical treatment in Venezuela.
The first shipment of humanitarian aid finally entered the country on April 16th. That same month, Human Rights Watch published a detailed report about the status of our humanitarian crisis, alongside their recommendations. It was the first time that severe observations about the government’s role in the crisis had been issued by an international organization, with commentaries to the UN like “(it’s necessary to) eliminate obstacles for a large-scale humanitarian operation,” something unattended to this day. On November 25th, the Venezuelan Pediatrics Association condemned the politicization of humanitarian supplies’ distribution for the nutritional recovery of children.
In May, we saw another issue of the “Amenaza triple” report by the International Council of AIDS Service Organizations (ICASO) and Acción Ciudadana Contra el SIDA (ACCSI.) Among their findings, there’s a concerning increase of measles (5,525 cases in 2018,) the decline of every indicator measuring health, poverty, nourishment and economic growth, and an increase in the figures of tuberculosis, malaria and people living with untreated HIV.
Even though the Global Fund approved the budget to send humanitarian aid to Venezuela on September 2019 (under the framework established on the Plan Maestro,) there’s no record of the antiretrovirals distributed up until the moment this report was published.
The National Hospital Survey issued two more reports. The first one, in July, was focused on the operativity of critical areas and supply shortage. It was especially important because it gathered the effects of the energy crisis, finding a small improvement on the shortage index (that could probably be attributed to the entry of humanitarian aid,) even though in most cases the shortages were around 50% in emergency rooms and 35% in ORs.
They could also see the disparity between distribution to hospitals in different areas of the country, like centers of reference in Merida, Monagas and Trujillo as the most unfavored.
They arrived to the conclusion that ORs operativity was tied to the availability of basic services, like water and power. The norm should be 100% availability of both, 365 days a year. Between March and April, they registered 32 deaths with powercuts as the direct cause.
In the second issue of the survey, covering until September, they evaluated the operativity of hospital aid services (X-rays, CT scans, labs), dialysis services and emergency human resources. Hospital aid services had availability well below what’s necessary to keep the main hospitals in the country running; X-rays had a 58% availability in the country between November 2018 and September 2019; Lab service was 55% unavailable and CAT scans, 85.6%. All of this has a direct impact on the ability to make a diagnosis in hospitals of reference all around the country.
Dialysis availability in Venezuela affects thousands of patients and 18% of hospitals didn’t have it. Regarding the human component, there’s no significant difference in emergency services, even though there’s a decreasing trend in nurse availability.
In addition to the National Hospital Survey findings, November brought other concerning news that show the deplorable state of public health in Venezuela. On the 13th, the National Hygiene Institute confirmed that a sample collected in September came out positive for yellow fever. The Venezuelan territory is now at risk with the first case confirmed since 2005, diagnosed in Bolívar. An irrefutable sign of unacceptable vaccination coverage.
Dialysis availability in Venezuela affects thousands of patients and 18% of hospitals didn’t have it.
The WHO’s World Malaria Report was issued recently, too. Last year, 750,000 new suspected cases of malaria were reported in Venezuelan territory, most of them in Bolívar. 453,000 of these were confirmed, representing a 51% of all cases reported in the hemisphere.
A year with a promising start ends full of uncertainty. Living conditions are worse every day, with children passing out from hunger in schools (Cáritas de Venezuela reports 13.5% severe malnutrition in kids under 5) and dying in hospitals while they wait for cancer treatment. Decades of public health work have been lost. The state continues to refrain from providing official figures or taking responsibility for their terrible management, and hundreds of families endure the hardships of having chronically ill relatives in a country plagued by hyperinflation and shortages.
The damage the dictatorship has inflicted on us will never be compensated. The loss is measured in lives.
Caracas Chronicles is 100% reader-supported.
We’ve been able to hang on for 22 years in one of the craziest media landscapes in the world. We’ve seen different media outlets in Venezuela (and abroad) closing shop, something we’re looking to avoid at all costs. Your collaboration goes a long way in helping us weather the storm.
Donate




